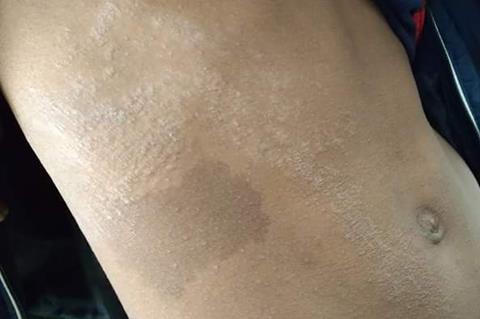
Lichen striatus (LS), a skin condition manifesting as linear eruptions following Blaschko’s lines on the trunk or limbs of children, is often accompanied by hypopigmentation (loss of melanin or skin color).
Interestingly, LS has a higher frequency of hypopigmentation compared to that of other skin inflammations, with up to 50% cases that can persist for several months to even years. However, the cause behind this trend is not clear.
The gram-positive bacterium Cutibacterium acnes has previously been associated with various skin conditions, including acne vulgaris and post-inflammatory hypopigmentation. There could, therefore, be a potential association between C. acnes and the observed skin microbiota of patients with LS with and without hypopigmentation.
Detailed study
With this hypothesis, a team of researchers from Korea led by Associate Professor Yun Hak Kim from the Department of Anatomy and the Department of Biomedical Informatics and Professor Hyun-Chang Go from the Department of Dermatology, both at Pusan National University, recently conducted a detailed study to ascertain this relationship. Their paper was published in the Journal of the European Academy of Dermatology & Venereology on 3 January 2024.
They collected and analyzed skin samples of 18 patients with LS (11 with hypopigmentation and 7 without it) confirmed by biopsy through whole genome sequencing and performed bioinformatics analyses to assess microbial differences in them. Despite the diverse stages of LS in patients with hypopigmentation, significant differences were observed in their skin microbiomes. This observation suggested a strong association between LS hypopigmentation and the skin microbiome.
Comparing patients with LS with and without hypopigmentation, the researchers discovered a quadrupled presence (23.26% versus 5.29% of the entire microbiota) of Cutibacterium acnes in the former.
Bacterial community
“Through network analysis between various microbial species found in the skin samples of patients with LS, we observed that C. acnes significantly influenced the bacterial community in hypopigmented LS, holding a central position in relationships with other bacteria. It further strengthens its potential association with LS hypopigmentation pathogenesis,” highlights Dr. Kim.
The research team additionally identified Malassezia, a genus associated with hypopigmentation in other skin disorders, in abundance among patients with LS with hypopigmentation (0.58% versus 0.31% of the entire microbiota). This finding, in particular the presence of Malassezia restricta, points at a potential link between Malassezia and LS hypopigmentation for targeted future research. Furthermore, Comamonas (15.29% versus 13.45% of the entire microbiota) and Aspergillus (0.30% versus 0.26% of the entire microbiota) were identified as other likely candidates.
Skin microbiota
Overall, there is likely a relationship between imbalance in the skin microbiota and LS-associated hypopigmentation. The frequency of Malassezia and C. acnes in hypopigmented LS cases suggests that these two conditions could be novel treatment targets for reducing LS duration as well as hypopigmentation. Patients with LS could thus lead a better quality of life if targeted therapy is focused on these microbiological components.
Future studies exploring temporal changes in the microbiome and observing the effects of antibiotic or antifungal agents on hypopigmentation frequency and duration could offer valuable insights into causative or correlative relationships between microbiome alterations and LS hypopigmentation.
“Our findings provide promising avenues for further research to decipher the relationship between skin microbiota and LS hypopigmentation, ultimately aiming to elucidate novel therapeutic strategies,” concludes Dr. Kim.






No comments yet