Animal models are a necessary research tool for understanding how diseases develop and how therapies work in biological systems and can be credited for breakthroughs ranging from effective antibiotics to the COVID vaccines.
The responsible and judicious use of animal models is prioritized by research institutions around the world and a unique research protocol developed by Melanie Pearson, Ph.D., of the Department of Microbiology & Immunology, and her team at University of Michigan Medical School is garnering widespread interest among microbiologists.
In a recent paper in the journal Infection and Immunity, her group describes a product called organ agar that could be deployed to more efficiently screen bacteria that cause urinary tract infections.
Strange concoction
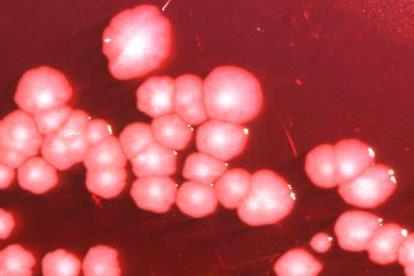
Agar is a gelatinous product made of seaweed routinely used in laboratories to grow colonies of bacteria in petri dishes.
Pearson discovered that creating a mixture composed of the agar plus human urine and the organ her team wanted to study, specifically the bladder and kidneys, enabled their team to screen more than 1,700 mutants of the UTI-causing bacteria Proteus mirabilis using a quarter of the mice typically required.
Pearson explains that in a classic mouse study of a urinary tract infection, mutated bacteria - bacteria that are missing individual genes - are introduced into an animal’s bladder and then the dominant strains assessed to determine what bacterial genes are important for infection. Knowing this could enable researchers to target specific variants for drug development, for example.
Bottleneck problem
The use of organ agar has multiple potential benefits, explains Pearson. For one, it can help microbiologists get around what is known as the bottleneck problem.
In a living system, only a certain number of mutants are able to gain a foothold, with the rest lost at random. When Pearson tried the screening method using organ agar, her team found that the dominant bacteria reproduced those that were dominant in a live animal.
What’s more, bacteria that did not do well on organ agar also did not do well in a live animal.
Furthermore, organ agar could enable researchers without access to animal models to create physiologically relevant models of infection or colonization and allow for more efficient screening of bacterial and other microorganism candidates for further study.
Paper cited: “Organ agar serves as physiologically relevant alternative for in vivo bacterial colonization,” Infection and Immunity.







No comments yet