The climate emergency poses a major threat to human health. Rising temperatures and changes in ecosystem conditions, coupled with globalisation and human action, such as the extensive use of fungicides and antibiotics in agriculture, can favour the emergence and spread of new species of hitherto underestimated potentially virulent pathogenic microorganisms, such as fungi.

An understanding of the evolutionary routes these potential pathogens have followed, how they have acquired their virulence, or how they have developed the capacity to infect humans is key to being able to monitor them and prevent future deadly epidemics, such as the recent COVID-19 pandemic, caused by the emergence of the SARS-CoV-2 virus.
A team from the Institute for Research in Biomedicine (IRB Barcelona) and the Barcelona Supercomputing Center - Centro Nacional de Supercomputación (BSC-CNS), led by the ICREA researcher Dr. Toni Gabaldón, has now identified a fungus from the Candida family as a potential pathogen. The Candida fungus family are microorganisms that cause infections such as vaginal candidiasis or systemic candidiasis, which can be fatal for immunocompromised people.
Hybrid microorganism
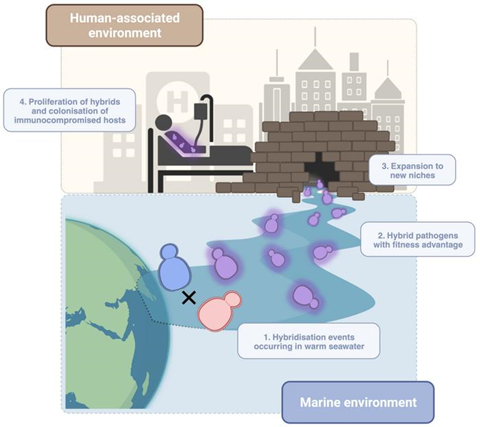
The team of researchers has discovered that Candida orthopsilosis is a hybrid microorganism that originated from two other parental fungi in a marine environment. And it is precisely this hybridisation that has conferred certain properties, such as the capacity to infect the human body and also virulence, which make it a potential threat to global health.
Published in the journal Nature Communications, this finding also paves the way for identifying the adaptations that allow certain microorganisms to be more likely to colonise humans and cause disease.
“We have spent years trying to answer the question of what makes some species pathogenic for humans and others, such as those we have in our microbiome, not,” says Dr. Gabaldón.
“Our results show that hybridisation—a process that has received little attention so far— allows the rapid acquisition of properties that allow human infection. Therefore, in fungi, this process could be a shortcut to conquer a species like ours,” he adds.
Cinematic infection
With due caution, this is the plot of the recent and popular miniseries “The Last of Us” (HBO Max), in which a fungus quickly acquires an enormous capacity for infection, transmission, and virulence, a perfect cocktail of properties which allows it to decimate humanity in a short time.
It is estimated that there are currently more than one million species of fungi, most of which are adapted to live in temperate or low temperatures in the soil, the aquatic environment, trees and plants, and animals such as amphibians, fish, reptiles, and insects.
Since the 1980s, the number of outbreaks of emerging infectious diseases has risen by nearly 7% per year, and fungi are increasingly being identified as a major threat to public health worldwide. And the increase in global temperatures has made them tolerant to warm environments, including the human body.
This is the case of Candida auris, a fungus that has adapted to be able to infect people, that is also potentially multi-drug resistant and can spread efficiently in hospital environments. There have already been hundreds of outbreaks of this infection worldwide, with a mortality rate of between 30 and 60%. Scientists point out that it could be the first microorganism that has become a pathogen as a result of climate change.
Better adapted hybrids
The same could happen with C. orthopsilosis. Dr. Gabaldón and his team have studied nine yeast samples isolated from the marine environment, specifically on the coast of Qatar, in the Arabian Sea. The researchers have sequenced and analysed their genomes and found that most of the fungi found are hybrids. This observation has led them to hypothesise that these fungi might have undergone adaptations that give them an advantage over their parental strains.
Likewise, they have found that these microorganisms from the marine environment are closely related to those they have found in clinical samples. Given these observations, they indicate that the hybridisation and emergence of this new microorganism must have occurred in the sea and, from there, moved to the humans, causing health issues. How it did this is still a mystery.
“Our results show us that the genetic characteristics that make the hybrids competitive and able to survive in the marine ecosystem could be advantageous for doing the same in humans,” says Dr. Gabaldón.
Optimal temperature
All the marine samples in the study were isolated in subtropical waters with temperatures between 35°C and 44°C. “We saw that the optimal temperature at which strains of C. orthopsilosis grow is 35°C and that they could survive up to much higher temperatures. This observation is worrying because their tolerance surpasses the thermal barrier of mammals, which until now had acted as a protective shield, and paves the way for infecting humans,” adds Dr. Valentina del Olmo, postdoctoral researcher in Dr. Gabaldón’s group and first author of the study.
Dr. Gabaldón adds that these are opportunistic pathogens that usually infect immunocompromised people, such as cancer patients, HIV patients, the elderly, and newborns, among others, a group that is growing in number.
The researchers conclude: “With the continuous increase in global temperatures and the overuse of antifungal drugs in agriculture and clinical practice, the appearance of fungi in the environment capable of overcoming the thermal barrier of mammals, acquiring resistance to fungicidal drugs and becoming a potential threat will increase.”







No comments yet