A novel therapeutic strategy developed by researchers at São Paulo State University (UNESP) could revolutionize the treatment of visceral leishmaniasis, a neglected tropical disease (NTD) transmitted by sandflies.
Some 12 million people suffer from the disease worldwide, and 700,000 to 1 million new cases of occur annually, according to the World Health Organization (WHO).
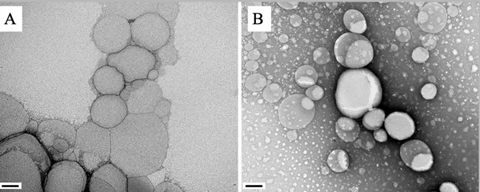
The technique developed by the researchers involved the use of lipid nanoparticles to administer lupeol, a chemical compound known to kill the Leishmania protozoan parasites that cause the disease. Lupeol is a triterpene found in many vegetables and fruits, including mangoes, grapes and strawberries, green peppers and olives, for example.
In animal tests, the strategy proved capable of eliminating Leishmania from affected organs. The results are reported in an article published in the journal Pharmaceuticals.
Visceral form
There are three main forms of leishmaniasis. The visceral form is the most serious, with a mortality rate of up to 95% if untreated, and up to 10% even when treated, according to WHO. The others are cutaneous leishmaniasis (the most common, usually causing skin ulcers), and mucocutaneous leishmaniasis (affecting mouth, nose and throat).
The available treatments – based mainly on the use of pentavalent antimonials or amphotericin B – have severe side effects, affecting particularly the heart, liver and kidneys. Some leishmaniasis drugs are extremely expensive, constituting a heavy burden for public health systems, and may create drug resistance in the parasite if administered inadequately. The researchers, therefore, stress in the article the urgent need to find or develop novel active compounds, including some identified in plants.
Novel technique
In the study, which was funded by FAPESP, researchers affiliated with the Institute of Biosciences on UNESP’s Coastal Experiment Campus (IB-CLP) in São Vicente created a novel technique that consisted of delivering lupeol in lipid nanoparticles.
“Lupeol has been shown in vitro to be capable of eliminating forms of Leishmania, but it isn’t very soluble in physiological solutions, which limits its bioavailability in vivo,” said Jéssica Adriana de Jesus, first author of the article and a postdoctoral researcher at IB-CLP-UNESP.
“Putting it in lipid nanoparticles solves the problem by surmounting biological barriers, maximizing therapeutic effect and delivering the medication to the targets, which in the case of visceral leishmaniasis are the spleen, liver and bone marrow. The nanocarriers are simply the delivery vehicle. When they reach the target site, with the right pH they open up and release the medication.”
First time ever
The experiments involved four groups of hamsters infected with Leishmania infantum and treated for ten days. The first group was given lupeol only, the second received nanoparticles containing lupeol, the third was given empty nanoparticles, and the fourth received placebo only. Samples were then taken from the animals’ spleen, liver, blood and plasma for biochemical, physiopathological and parasite load analysis.
As expected, the lipid nanoparticles carrying lupeol were more effective than lupeol alone in eliminating visceral leishmaniasis parasites from the spleen and liver: administration of the nanoparticles with lupeol for ten days reduced the number of parasites by 99.9%.
“In addition, the animals treated in this way exhibited minimal histopathological alterations in the spleen and liver. For the first time ever, we proved that this combination is highly effective in treating the disease and is a significant formulation whose use should be considered.”
Developing a nanocarrier
The nanoparticles containing lupeol were administered by intraperitoneal injection. The group now plans to develop a nanocarrier for oral administration, which would enable the patient to take the medication at home, as well as versions for topical treatment of cutaneous leishmaniasis.
The study was conducted during Jesus’s postdoctoral fellowship and supervised by Luiz Felipe D. Passero, last author of the article. Passero is a professor at IB-CLP-UNESP and at the Institute for Advanced Marine Studies (IEAMar-UNESP), also in São Vicente.
The other co-authors are Ilza Maria O. Sousa, State University of Campinas (UNICAMP); (Unicamp); Thays Nicolli, Aurea F. Ferreira and Marcia D. Laurenti, Infectious Disease Pathology Laboratory, Hospital das Clínicas (HC), the hospital complex run by the University of São Paulo’s Medical School (FM-USP); and Domingos C. Ferreira and Paulo C. Costa, Pharmaceutical Technology Laboratory, University of Porto (Portugal).
Topics
- Aurea F. Ferreira
- Disease Treatment & Prevention
- Domingos C. Ferreira
- Ilza Maria O. Sousa
- Infectious Disease
- Innovation News
- Jéssica Adriana de Jesus
- Leishmania infantum
- lipid nanoparticles
- Luiz Felipe D. Passero
- lupeol
- Marcia D. Laurenti
- Paulo C. Costa
- São Paulo State University
- State University of Campinas
- Thays Nicolli
- The Americas
- University of Porto
- Veterinary Medicine & Zoonoses
- visceral leishmaniasis







No comments yet