A global wave of infections caused by fungi growing drug-resistant has the medical community issuing precautions on how to protect yourself.
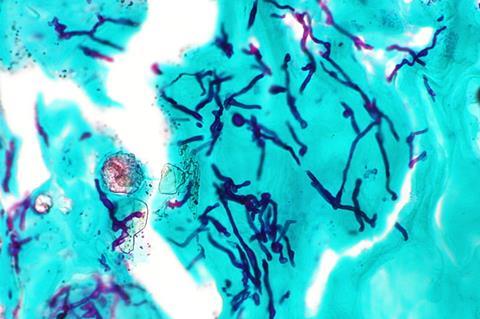
Skin contact with microorganisms found in soil or on hard surfaces, such as common shower facilities, or exposure to infected pets, can result in fungal infections known as dermatomycoses. Rashes, itching, burning and skin irritation are among the symptoms.
Epidemiological data published in Microbial Cell indicates that a rise in severe fungal infections has resulted in over 150 million cases annually and almost 1.7 million fatalities globally.
Rising antifungal resistance
In a recent study published in Pathogens and Immunity, Thomas McCormick and Mahmoud Ghannoum, professors of dermatology at the Case Western Reserve University School of Medicine and affiliated with University Hospitals Cleveland Medical Center, explain how rising antifungal resistance is worsening the problem of invasive fungal infections.
“This is not just an issue that affects individual patients,” McCormick said. “The World Health Organization has recognized it as a widespread threat that has the potential to impact entire healthcare systems if left unchecked.”
Based on their findings, the researchers issued precautions and a “call to action” for the medical community to help protect people from multidrug-resistant fungi—starting with awareness and education.
“Healthcare providers must prioritize the use of diagnostic tests when faced with an unknown fungal infection,” Ghannoum said. “Early detection can make all the difference in improving patient outcomes.”
Vulnerable patients
Patients treated with medications to protect the immune system after cancer and transplant procedures are more vulnerable to fungal infections—making them especially more vulnerable to infections from drug-resistant fungi, the researchers said.
The emergence of multidrug-resistant fungal species, such as Candida auris and Trichophyton indotineae, is especially troubling and requires urgent attention, they reported.
In a study recently published in Emerging Infectious Diseases, Ghannoum’s research team and the Centers for Disease Control and Prevention (CDC), detailed a case that demonstrated Trichophyton indotineae, in addition to becoming drug-resistant, was also sexually transmissible.
To address the growing health concern, McCormick and Ghannoum suggest several measures:
- Increased awareness and education: Raising awareness in the general healthcare setting to obtain a more accurate understanding of the rise of antifungal-resistant infections.
- Diagnostic Testing: Routine use of diagnostic tests can guide appropriate treatment strategies.
- Antifungal Susceptibility Testing (AST): Improving insurance reimbursement rates for AST and increasing the number of qualified laboratories with the capacity to perform these tests.
- Call to Action: Addressing the emerging challenge of antifungal resistance involves concerted efforts from healthcare professionals, researchers, policymakers and the pharmaceutical industry to develop and implement strategies for managing and preventing antifungal resistance.
“The ultimate goal of these measures,” Ghannoum said, “is to improve the quality of patient care by ensuring effective treatment and preventing further escalation of the problem.”







No comments yet