Yale researchers have discovered that one of the most abundant beneficial species found in the human gut showed an increase in colonization potential when experiencing carbon limitation — a finding that could yield novel clinical interventions to support a healthy gut. The findings were published March 16 in Science.
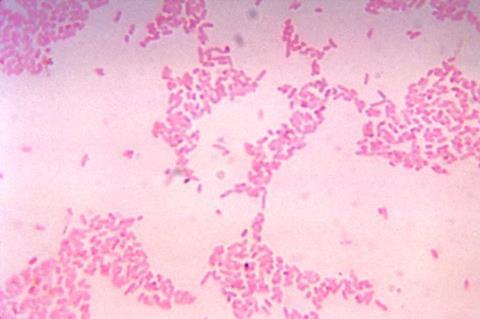
The Yale team, based in the lab of geneticist Eduardo Groisman, the Waldemar Von Zedtwitz Professor of Microbial Pathogenesis, found that the beneficial gut bacterium Bacteroides thetaiotaomicron responded to starvation for carbon — a main building block for all cells — by sequestering a portion of the molecules for an essential transcription factor within a membrane-less compartment.
The team established that sequestration of the transcription factor increased its activity, which modified the expression of hundreds of bacterial genes, including several that promote gut colonization and control central metabolic pathways in the bacterium. These findings reveal that “good” bacteria use sequestration of molecules into membrane-less compartments as a vital strategy to colonize the mammalian gut.
Colonization factors
Bacteroides thetaiotaomicron and other bacteria residing in the mammalian gut have access to nutrients ingested by the host animal. However, there are also long periods of time when the host organism does not eat. Deprivation of nutrients, including carbon, elicits the production of colonization factors in beneficial gut bacteria, the researchers found.
“One of the things that emerged is that when an organism is starved for carbon, that is the signal that helps produce properties that are good for surviving in the gut,” said Aimilia Krypotou, a postdoctoral fellow in Groisman’s lab and lead author of the study.
A confluence of observations from the lab’s previous research led to the breakthrough. The first was when Groisman noticed that the size of the transcription factor from the gut microbe was much larger than those of other well-studied homologous proteins from other bacterial species. The team then found that bacteria could not survive in the gut of a mouse without the extra region absent from homologous proteins.
Extra region
Krypotou then hypothesized that the extra region might confer a new biophysical property to the transcription factor required for the bacteria to survive in the gut, and successfully performed a series of experiments to test the hypothesis.
An awareness of these membrane-less compartments actually goes back a hundred years, Groisman said. Krypotou’s key insight, he said, was to deduce novel properties for the bacterial transcription factor — termed Rho — based on the extra region. Sequestration of the transcription factor takes place by a process known as liquid-liquid phase separation, a ubiquitous phenomenon present in a wide variety of cells including those of humans.
“This phenomenon has been known but is usually associated with stress in eukaryotic organisms, such as plants, animals, and fungi,” said Groisman. “Recently it was realized it can also happen with bacteria and, in our case, we established that it occurs in commensal gut bacteria, which require it for survival in the gut. One could conceivably, potentially imagine that if one were to manipulate organisms prone to this effect, perhaps one could improve organisms beneficial to humans.”
The findings could help spur the development of new probiotic therapies for gut health, Krypotou said.
“Most studies just look at abundance of bacterium,” she said. “If we don’t understand what’s happening at the molecular level, we don’t know if it would help.”
Other authors include Guy Townsend III and Xiaohui Gao, former postdoctoral fellows; Nick Pokorzynski, current postdoctoral fellow in Groisman’s lab; Jun Liu and Shoichi Tachiyama, postdoctoral fellow in Liu’s lab, and Andrew Goodman from Yale Microbial Sciences Institute.





No comments yet