Pneumonia is an infection of the lung alveoli caused by bacteria, viruses or fungi. It is one of the leading causes of morbidity and mortality worldwide, representing a clinical and economic burden and a global public health problem.
The microbial ecosystem (or microbiome) of the human respiratory tract colonizes different niches. The respiratory tract microbiome is of interest to scientists as it contributes to human health by stimulating the immune system and protecting against infection by pathogens.
Scientists from the Institut Pasteur and the CNRS have demonstrated that the microbiome composition, pathogen load and clinical interventions influence the severity of bacterial pneumonia caused by Legionella pneumophila. The results were published in the journal Cell Reports Medicine on August 25, 2023.
Respiratory tract microbiome
In this study, scientists from the Biology of Intracellular Bacteria Unit, led by Carmen Buchrieser at the Institut Pasteur, in collaboration with Sophie Jarraud, Head of the National Reference Center for Legionella in Lyon, analyzed the diversity and composition of the respiratory tract microbiome (bacteria, archaea, fungi and protozoa) in patients with pneumonia caused by the intracellular bacterial pathogen Legionella pneumophila for their entire hospitalization period.
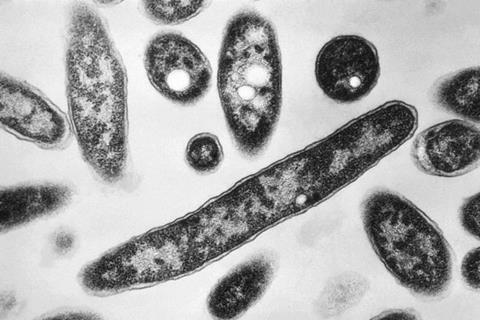
L. pneumophila is responsible for a severe pneumonia known as Legionnaires’ disease, which can be contracted by inhaling contaminated aerosols from artificial water sources such as showers, hot tubs or air conditioning systems.
The fatality rate for Legionnaires’ disease varies from 5 to 40% depending on the clinical context and the region. Risk factors are old age, pre-existing lung conditions, smoking and immunosuppression, and around two-thirds of reported cases occur in men.
Rising cases
Confirmed cases of Legionnaires’ disease in the European Union went from 4,693 cases in 2005 to 10,004 cases in 2021, an increase of 113%. One of the reasons for this sharp rise may be climate change, with higher water temperatures and more frequent and intense floods that allow Legionella to replicate more rapidly and to access human environments.
The team of scientists combined high-throughput bacterial, archaeal and fungal marker gene sequencing with a quantification approach to characterize how the respiratory tract microbiome developed in patients over the course of infection and as a result of hospital-related interventions (such as mechanical ventilation and administration of antibiotics).
A unique cohort of 38 hospitalized patients with pneumonia caused by Legionella pneumophila was analyzed.
Complex dynamics
“We discovered complex microbiome dynamics, where commensal and pathogenic microorganisms coexist, and the equilibrium among their abundance drives the microbiome to recovery or dysbiosis,” explains Carmen Buchrieser, lead author of the study and Head of the Institut Pasteur’s Biology of Intracellular Bacteria Unit.
The scientists observed that early in hospitalization, microbiome diversity decreased and the pathogen L. pneumophila was killed by the antibiotic treatment. But the empty niche was soon occupied by other opportunistic species, often resistant to antimicrobials – a factor that should be considered in prevention strategies for secondary infections.
The respiratory tract microbiomes with the highest bacterial and fungal loads also showed lower diversity and pathogen enrichment, indicating that high biomass could be a biomarker for secondary and/or co-infections.
Biomass link
Finally, the scientists showed that Legionella biomass correlates with disease severity and comorbidities, suggesting that pathogen quantification should be included in patient monitoring. Clinical interventions such as mechanical ventilation or administration of certain types of antibiotics influence the microbiome composition and therefore also disease outcome.
“In this study we also discovered that fungi, archaea and protozoa may be resident and not merely transitory in the respiratory tract of hospitalized patients and that they might contribute to pneumonia progression. This requires further investigation. Our research therefore shows that the interaction between respiratory tract microbiome equilibrium, pathogen load dynamics and clinical interventions plays a crucial role in the recovery of patients with pneumonia,” concludes Carmen Buchrieser.







No comments yet