An international clinical trial co-led by UCL (University College London) researchers will evaluate much-needed new antibiotic combinations for newborn babies with sepsis.
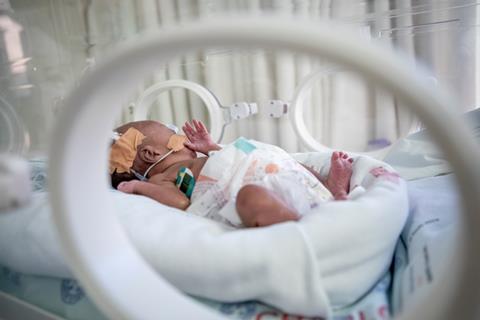
The trial, which has started in three public hospitals in South Africa and Kenya, will be expanded to other countries and regions in 2024, with a target of recruiting up to 3,000 newborns overall.
The NeoSep1 trial will evaluate new combinations of generic antibiotics and compare them to existing treatment regimens that are often used in newborn babies with suspected neonatal sepsis.
Chris Hani Baragwanath Academic Hospital in Johannesburg, Tygerberg Hospital in Cape Town and KEMRI, Kilifi County Hospital in Kenya are involved in the initial stage of the clinical trial.
Resistant infections
Neonatal sepsis, a life-threatening infection, affects up to 3 million babies a year globally. It has become increasingly challenging as about 40% of infections are reported to be resistant to standard antibiotic treatments. Over 214,000 newborn babies die of drug-resistant neonatal sepsis every year, mostly in low- and middle-income countries (LMICs).
The trial is sponsored by the Global Antibiotic Research and Development Partnership (GARDP) in collaboration with the Medical Research Council Clinical Trials Unit at UCL (MRC CTU at UCL); St George’s, University of London; and Penta.
“Many babies are dying because of limited treatment options. The NeoSep1 trial is an opportunity to shift this trajectory by identifying new antibiotic combinations that we can tailor to treat neonatal sepsis in settings where there is widespread resistance to current recommended options. This is vital if we are going to address the impact of antimicrobial resistance on the burden of disease related to neonatal sepsis,” said Seamus O’Brien, Director of Research and Development at GARDP.
Ranking combinations
The trial will rank the safety and efficacy of three new combinations of older antibiotics (fosfomycin-amikacin, flomoxef-amikacin, and flomoxef-fosfomycin) against the current standard of care. It will also assess and validate the doses of two antibiotics (fosfomycin and flomoxef) for use in newborns.
A key goal is to find out whether some antibiotic treatments perform better than others for the empiric treatment of babies with neonatal sepsis, particularly in LMICs where highly resistant bacteria are common. The trial will also consider how these combination treatments can best be used in hospital settings with varying levels of antibiotic resistance.
A new way of comparing antibiotic treatments with each other, called the Personalised Randomised Controlled Trial (PRACTical) design, will be used. The novelty of this design is that it allows researchers to compare many antibiotic treatments for neonatal sepsis. It will also enable doctors to choose treatment regimens that are likely to work well for newborns in their particular hospital settings.
“The development pipeline for new antibiotic treatments is limited and the lack of a universal, effective standard of care creates huge challenges in conducting research to tackle neonatal sepsis. Novel trial designs such as the PRACTical design have been specifically developed to address these challenges in important public health emergencies such as neonatal sepsis,” said Sarah Walker, Professor of Medical Statistics and Epidemiology at the MRC CTU at UCL.
Global study
The NeoSep1 trial builds on findings from a global observational study of sepsis in newborn babies, conducted by GARDP and partners in 19 hospitals in 11 countries from 2018 to 2020. GARDP published a report on the study in 2022.
The study found a worryingly wide variation in treatment and frequent switching of antibiotics because of high resistance to treatments.
“Newborns handle medicines very differently to older infants, children and adolescents. Premature or otherwise critically ill babies are at great risk of severe infection or sepsis because of their immature immune systems. The types of bacteria causing newborn infections are not necessarily the same as those found in other patients. For these reasons, it is essential to investigate antibiotic treatments of newborns with sepsis,” said Dr Julia Bielicki, paediatrician and researcher in the Centre for Neonatal and Paediatric Infection at St George’s, University of London.
The trial aims to generate relevant and reliable evidence for doctors who need to make treatment decisions, especially in hospitals where there are high levels of antimicrobial resistance.
Last resort
“We often have to treat babies with a combination of the antibiotics of last resort. On top of this we are not 100% sure about how to dose these drugs. We’re dealing with fragile newborns, so we need to be aware of the potential toxicity of the antibiotics and dosages we use. This trial will help in giving us confidence that we are delivering more effective treatment. This is critical as we want the best possible outcome for newborns in our care,” said Adrie Bekker, Principal Investigator for the NeoSep1 trial at Tygerberg Hospital, Cape Town, and Professor in the Division of Neonatology, Department of Paediatrics and Child Health at Stellenbosch University.
“We need to treat newborn babies in our care promptly and effectively otherwise there is great risk that babies could die or are left with neurodevelopment impairment. Having the right antibiotics can make the difference between life and death. We are hoping the trial will provide robust evidence that the antibiotic combinations are safe and effective and that this will lead to a change in both WHO and local treatment guidelines,” said Christina Obiero, Principal Investigator for the NeoSep1 trial for the KEMRI-Wellcome Trust Research Programme at Kilifi County Hospital, Kenya.
Topics
- Adrie Bekker
- Chris Hani Baragwanath Academic Hospital
- Christina Obiero
- Infection Prevention & Control
- Julia Bielicki
- Kilifi County Hospital
- Middle East & Africa
- neonates
- One Health
- Penta
- Personalised Randomised Controlled Trial
- Research News
- Sarah Walker
- sepsis
- St George’s, University of London
- Stellenbosch University
- Tygerberg Hospital
- UK & Rest of Europe
- University College London






No comments yet