A comprehensive investigation published in Science in One Health has identified a previously underappreciated source of thermotolerant Campylobacter spp. in South American camelids (SACs)—alpacas and llamas kept in Germany. The findings underscore the importance of expanding epidemiological surveillance beyond traditional livestock to encompass emerging animal husbandry practices in addressing foodborne pathogen transmission.

While Campylobacter jejuni remains the leading bacterial cause of gastroenteritis globally, and thermotolerant Campylobacter species are established zoonotic pathogens associated with conventional livestock, their prevalence and characteristics in SACs—a growing sector in European animal agriculture—have received scant scientific attention. This knowledge gap prompted a systematic examination of Campylobacter presence in these animals.
Fecal samples
Researchers collected 717 fecal samples from alpacas and llamas across multiple seasons, employing molecular typing and virulence profiling to characterize any isolates recovered. The results revealed Campylobacter spp. in 23 samples (3.2% prevalence), comprising 16 Campylobacter jejuni and 7 Campylobacter coli isolates. Notably, alpacas exhibited substantially higher infection rates (4.9%) compared to llamas (0.7%), indicating species-specific differences in bacterial colonization.
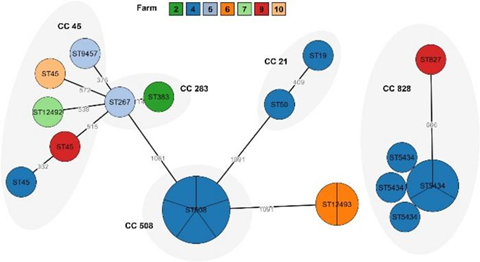
Seasonal variation was evident, with elevated prevalence during summer months—a pattern consistent with observations in conventional poultry and cattle production systems. Molecular typing revealed significant genetic diversity, with multiple sequence types identified among the isolates. Several of these genetic signatures matched those previously documented in livestock and human clinical cases, suggesting potential pathways for cross-species transmission.
Virulence and resistance
All isolates harbored virulence-associated genes, confirming their pathogenic potential. Additionally, antimicrobial resistance was detected in a subset of isolates, including resistance to ciprofloxacin and tetracycline—antibiotics critical for clinical management of campylobacteriosis in humans.
These findings highlight an often-overlooked epidemiological blind spot in current monitoring frameworks. As SAC husbandry expands across Europe, including in Germany, the animals’ capacity to harbor and potentially transmit virulent, genetically diverse Campylobacter isolates cannot be disregarded. The presence of antimicrobial resistance further elevates public health concerns.
The study underscores the relevance of a One Health approach—integrating veterinary, environmental, and human health perspectives—in comprehensively understanding foodborne pathogen epidemiology. Enhanced biosecurity measures, targeted monitoring, and improved understanding of transmission pathways from SACs to humans and food systems are essential to mitigate risks.
Research implications
The investigation advocates for:
- Expanded surveillance of thermotolerant Campylobacter spp. in non-traditional livestock species
- Evaluation of transmission routes from SACs to human populations and food chains
- Implementation of evidence-based biosecurity protocols specific to SAC operations
- Integration of emerging animal production systems into public health monitoring strategies
This research demonstrates how targeted epidemiological investigation can reveal previously unrecognized disease reservoirs, informing more comprehensive and effective strategies for reducing foodborne illness in the broader human population.







No comments yet