A recently released prospective analysis of the first eight years of the Johns Hopkins Medicine-led Zero TB in Kids program shows that significant reduction of tuberculosis (TB) transmission and burden (the total impact of health problems — specifically death, morbidity and disability — on a population) among schoolchildren in high-burden areas can be achieved using existing TB screening, treatment and follow-up protocols.
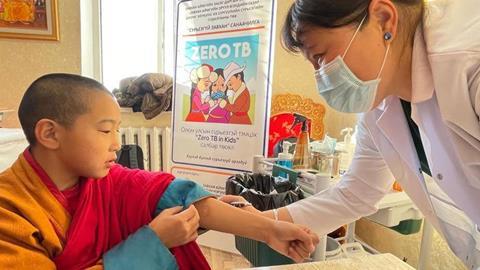
Since 2017, Zero TB in Kids, a comprehensive TB screening and tuberculosis preventive treatment (TPT) program, has been implemented in settings in northern India — such as schools, monasteries and nunneries — where Tibetan refugee schoolchildren congregate.
“To evaluate the effectiveness of the first eight years of our effort, we searched for studies published between January 2000 and December 2025 to compare the results of other TB screening and treatment programs with Zero TB in Kids,” says Kunchok Dorjee, M.D., Ph.D., project director and principal investigator of Zero TB in Kids and assistant professor of medicine at the Johns Hopkins University School of Medicine.
“To our surprise, we could not identify any study published in that period that demonstrated meaningful reduction of TB on a population level, indicating that there are significant gaps in promoting the knowledge and experience needed to make large-scale TB screening and TPT programs work.”
Tibetan communities
Between 2017 and 2024, comprehensive and longitudinal TB screening and TPT programs were conducted by Zero TB in Kids in congregate settings of the Tibetan communities in northern India. The effort worked exceptionally well, says Dorjee.
“Over the eight-year period, screening and TPT led to an 83% reduction in TB incidence and a 32% reduction in the prevalence of latent TB infection among children, in spite of setbacks arising as a result of the COVID-19 pandemic,” he says. “And after one round of screening and TPT, the occurrence of new TB infections declined by 59% in the child population.”
“The prevalence of TB disease also declined substantially in participants who did not receive TPT, indicating an overall deduction of TB transmission in the population,” adds Dorjee. “In comparison, the annual reduction of global TB rates is around 2%.”
Incidence and prevalence
According to the World Health Organization (WHO), incidence measures the number of new cases of a disease that appear in a specific population over a defined period, and therefore, represents disease risk. Prevalence, says WHO, measures the total number of individuals in a population, both new and existing cases, who have a disease at a specific point in time. Prevalence defines the burden of a disease.
A latent TB infection occurs when a person acquires the TB pathogen — the bacterium known as Mycobacterium tuberculosis — but does not have symptoms and can still transmit it to others.
Dorjee says the COVID-19 pandemic lead to a resurgence of TB conversions (people developing a positive TB skin test who were previously negative) and TB disease among the schoolchildren followed, but declines returned once screening and TPT resumed in 2024.
Participants with seizures and hepatitis B, Dorjee adds, were less likely to receive TPT during the study period. He says the researchers believe this occurred because of physicians being uncertain or lacking confidence in TPT for these groups, or fearing liver toxicity or drug interactions if the treatment was administered.
Three recommendations
Dorjee says that the success of the Zero TB in Kids program, which emphasizes community-led screening and TPT, shows that rapid and sustained reduction of TB transmission and TB impact in high TB burden areas is possible with optimized use of existing medications, tools and protocols for TB control.
“Based on these findings, we recommend three things,” says Dorjee. “First, a shift in the approach of global TB control must be made to emphasize surveillance of TB infections and TPT implementation; second, mass screenings and TPT should be conducted across schools and other congregate settings in high TB burden areas to bend the TB epidemic curve toward elimination in children and adolescents; and third, guidelines are needed to implement TPT in people with comorbidities, such as hepatitis B and seizures, for improved uptake and acceptance of TPT.”
Study background
Along with Dorjee, the members of the research team from Johns Hopkins Medicine and the Johns Hopkins Bloomberg School of Public Health are Sheriza Baksh, Robert Bollinger, Richard Chaisson, Sangyal Dorjee, Jonathan Golub, Amita Gupta, Rachel Sadoff and Sourya Shrestha.
Team members from other institutions are Tenzin Dechen, Tenzin Dolker, Ugen Gyatso, Jiqme Kalsang, Tenzin Kalsang, Tenzin Khachoe, Dekyi Lhadon, Tenzin Namdon, Tsetan Dorji Sadutshang, Tenzin Tsomo, Tenzin Thinley, Sonem Topgyal, Tenzin Yangkyi from the Delek Hospital and the Central Tibetan Administration (India); Ravinder Kumar and Rajesh Sood from the National TB Elimination Program, National Health Mission (India); Vidya Mave from the Centre for Infectious Diseases in India, Johns Hopkins Medicine (India); Lobsang Tsering from the Department of Health, Central Tibetan Administration (India); and Zorba Paster from the University of Wisconsin-Madison.
Federal funding for the study came from the National Institutes of Health’s National Institute of Allergy and Infectious Diseases (NIAID) grant K01-AI148583. Additional funding was provided by the NIAID-Johns Hopkins Center for AIDS Research and private donations, foundations and philanthropies.
None of the authors have any conflict of interest disclosures to report.
——————————————————
NOTE: A podcast, produced by the journal and featuring Dorjee discussing this study, is available here.







No comments yet