The body’s immune reaction to increased levels of a toxic molecule, part of a bacterial species in the human gut, may reveal who is most at risk of developing lupus nephritis, according to a new study led by NYU Langone Health.
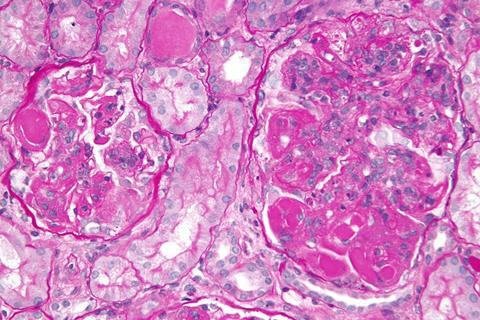
In people with the disease, which often leads to long-term kidney damage, the body’s immune system attacks its own tissues. Bouts of lupus nephritis have been tied by past studies to upticks in growth of the bacterial species Ruminococcus gnavus. This triggers excess production of the key molecule, a lipoglycan, which is a key part of the bacterium’s outer wall.
Ruminococcus gnavus and its lipoglycan, the researchers said, are present in the guts of healthy people without lupus, but at low levels when there is no growth of the species and no measurable immune response.
Led by NYU Langone researchers, the new work suggests that using antibiotics to target the Ruminococcus gnavus lipoglycan, or the toll-like receptor 2 (TLR2) protein it activates on immune cell surfaces to amplify damaging inflammation, could serve as an alternative to current lupus nephritis therapies that suppress the immune system.
Bacterial growths
Publishing in the journal Annals of the Rheumatic Diseases online April 23, researchers found Ruminococcus gnavus growths in half of a small group of female lupus nephritis patients. These patients with gut bacterial blooms all showed signs of inflammation and the presence of Ruminococcus gnavus antilipoglycan antibodies, leading the researchers to suspect that high levels of the molecule were a potential trigger or cause of the disease.
Further experiments in mouse models of lupus nephritis showed that exposing the guts of lupus mice to Ruminococcus gnavus triggered immune responses and inflammation, as well as serious renal damage similar to that seen in humans with the condition. Blocking toll-like receptor 2 (TLR2) in the lupus mice also dampened any lupus-linked inflammation.
READ MORE: Lupus flare-ups linked to Ruminococcus blautia gnavus blooms in gut
“Our study provides the foundational evidence that detection of antilipoglycan antibodies from Ruminococcus gnavus blooms in the gut could identify those people at increased risk of lupus nephritis,” said study senior investigator and immunologist Gregg Silverman, MD. Dr. Silverman is the Mamdouha S. Bobst Professor of Internal Medicine at the NYU Grossman School of Medicine.
Gut microbiome imbalances
“Our research reshapes our fundamental understanding of lupus nephritis, supporting our underlying theory that gut microbiome imbalances drive the disease, leading to Ruminococcus gnavus growths, which in turn produce the immune reactions and inflammation tied to long-term renal damage,” said Dr. Silverman, who is also a professor in the school of medicine’s Department of Pathology.
“Our findings also set the stage for using selective antibiotic drugs to block these bacterial growths, or other inhibiting drugs to block the toll-like receptor 2 toxins produced by these bacterial blooms, to treat lupus nephritis,” said Dr. Silverman.
Dr. Silverman said his team already has plans for clinical testing for anti-Ruminococcus gnavus lipoglycan antibodies as biomarkers for lupus nephritis. The team’s goal would be to stratify patients according to their risk of a microbiome-induced disease flare, potentially catching the disease when symptoms start to show.
“These results lay the groundwork for demonstrating how clinicians could diagnose and potentially treat lupus nephritis patients earlier and more effectively than before,” said Dr. Silverman.
Clinical trials
The researchers have also proposed clinical trials using anti-Ruminococcus gnavus lipoglycan antibodies or TLR2 chemical blockers to prevent or counter the effects of lupus nephritis flares. Such treatments could be much-needed alternatives, they say, to immunosuppressing drugs that are the current mainstay for lupus nephritis, and which do not work well for all. These therapies have side effects including weight gain, depression, and increased risk of infection.
According to the National Institutes of Health, lupus is much more common in women than in men, with lupus nephritis as the most potentially severe form of the disease. African Americans, Hispanics, and Asian Americans are all more likely to develop lupus nephritis than Caucasians. The number of Americans with lupus nephritis has more than doubled over the past 40 years, with 20% of all people with the disease developing end-stage kidney disease, which can be fatal.
Funding for this study was provided by National Institutes of Health grants R01AI143313, R21AI180737, and T32AR069515, with additional support provided by the Lupus Research Alliance and the Colton Foundation.
Background
Dr. Silverman and NYU Langone Health have patented intellectual property related to their latest research, including on tools to detect antilipoglycan antibodies and on treatments, based on antilipoglycan antibodies. NYU Langone Health is managing the terms and conditions of these relationships in accordance with its policies and procedures.
In addition to Dr. Silverman, NYU Langone Health researchers involved in this study are lead investigator Abhimanyu Amarnani, and co-investigators Cristobal Rivera, Macintosh Cornwell, Tyler Weinstein, Zakia Azad, Susan Gottesman, Cynthia Loomis, Andy Lee, Nimat Ullah, Joshua Prasad, Mingyang Yi, Kelly Ruggles, and Bhama Ramkhelawon.
Other study co-investigators are Laura Cooney at the University of Michigan in Ann Arbor, Brad Rovin at Ohio State University in Columbus, Laurence Morel at the University of Texas at San Antonio, Betsy Barnes at the Feinstein Institutes for Medical Research in New York City, and Nicolas Gisch at the Research Center Borstel, Leibniz Lung Center, in Germany.





No comments yet